Your healthcare software portals are driving NHS client complaints because fundamental technical problems are putting patients at risk and creating frustrating user experiences. This analysis is for healthcare IT leaders, NHS trust executives, and software vendors who need to understand why their systems are failing patients and staff.
NHS IT failures have become a patient safety crisis. BBC investigations reveal over 100 instances of serious harm linked to electronic patient records problems, with three confirmed deaths and 200,000 unsent medical letters across English hospital trusts. These aren't isolated glitches - they're systematic failures causing real harm.
Healthcare software user experience issues plague systems like Epic's MyChart portal, where patients struggle with inaccurate data, confusing authentication processes, and multiple conflicting identities across different trusts. Meanwhile, clinical staff report that critical patient information gets buried in poorly designed interfaces, leading to medication errors and missed diagnoses.
We'll examine the common technical problems creating patient safety risks, explore real cases where NHS software failures directly harmed patients, and analyze the user experience disasters driving complaint volumes. You'll also discover the hidden scale of these problems and why NHS digital transformation efforts keep falling short despite massive investment.
The evidence shows your current systems aren't just underperforming - they're actively dangerous. Patient portal technical problems and healthcare IT system failures demand immediate attention before more lives are lost.
Common Technical Problems Causing Patient Safety Risks
Poor integration between different NHS systems and apps
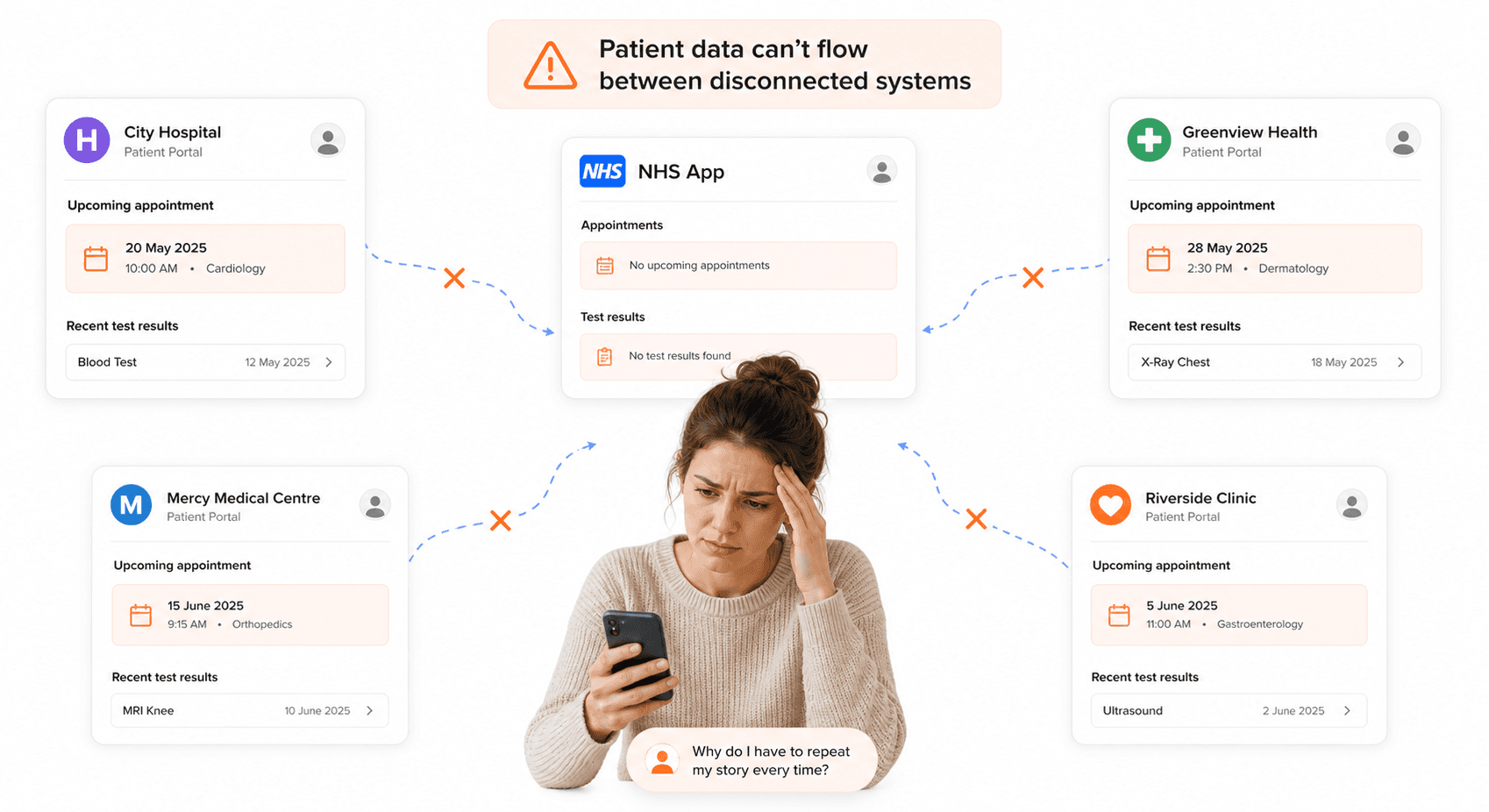
Your healthcare software portals are struggling with fundamental integration issues that directly threaten patient safety. The most glaring example involves the poor integration between Epic's hospital records portal and the NHS App, creating significant barriers for your patients trying to access their healthcare information. When you're dealing with US tech giant Epic's system, you're encountering compatibility problems that weren't adequately addressed during implementation planning.
These integration failures mean your patients cannot seamlessly transition between different NHS digital touchpoints. If you're using the NHS App to check your health records, you may find that critical information from hospital systems simply doesn't appear or appears incomplete. This fragmentation forces your patients to navigate multiple disconnected platforms, increasing frustration and reducing their confidence in NHS digital services.
The technical architecture underlying your healthcare software portals lacks the robust integration standards needed for modern healthcare delivery. Your IT teams are working with systems that weren't designed to communicate effectively, creating data silos that prevent comprehensive patient care coordination. This means when your clinicians need to access complete patient histories, they're often working with incomplete or outdated information.
Authentication failures preventing patient access
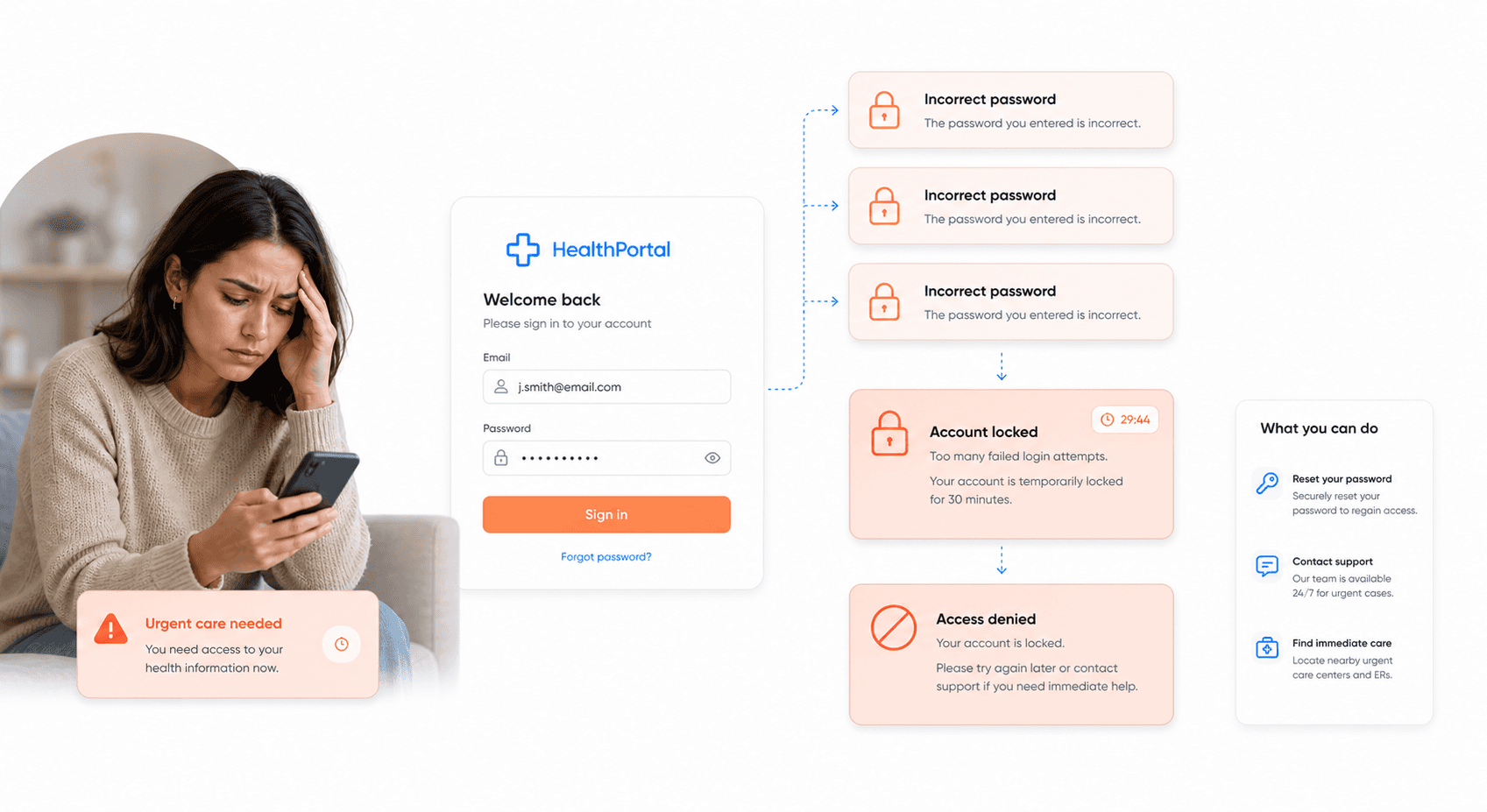
Your patients are experiencing significant authentication barriers that prevent them from accessing their own healthcare information when they need it most. Two-factor authentication issues are particularly problematic for systems like MyChart, where your users report being locked out of their accounts during critical health situations.
These authentication failures create a cascading effect on patient engagement with your healthcare software portals. When your patients cannot reliably access their health information, they lose trust in the digital systems and may revert to more traditional, less efficient methods of healthcare interaction. Your technical teams are dealing with authentication protocols that are either overly complex for patient use or insufficiently robust for healthcare security requirements.
The authentication problems you're facing extend beyond simple login issues. Your patients encounter scenarios where successful authentication doesn't guarantee access to all relevant health information, creating partial access situations that can be more dangerous than no access at all. These inconsistent authentication experiences undermine your digital transformation efforts and contribute directly to the volume of NHS client complaints you're receiving.
Critical patient information buried or invisible to clinicians
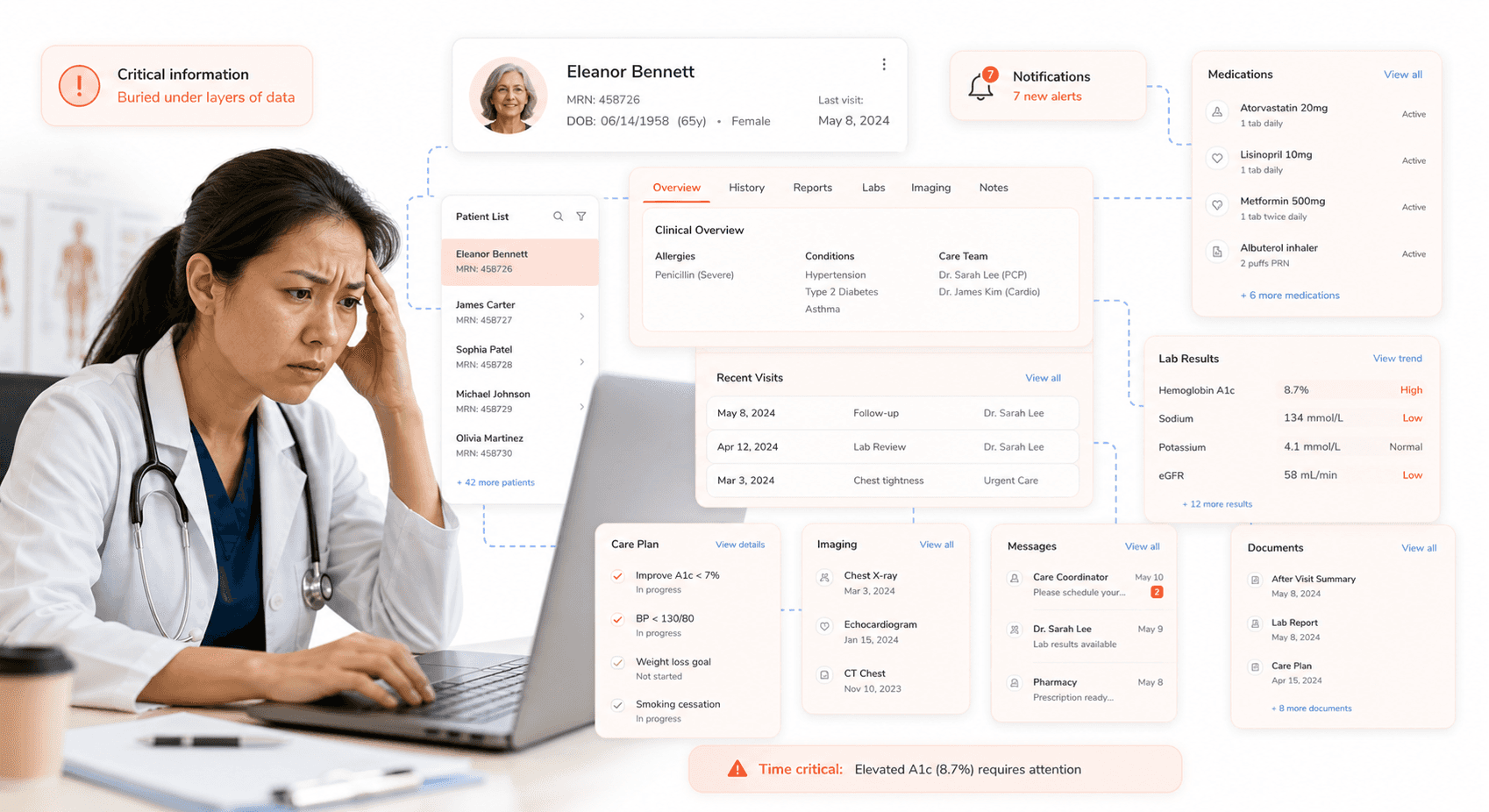
Your clinicians are reporting alarming difficulties in accessing critical patient information through healthcare software portals, with potentially life-threatening consequences. The case of Darnell Smith's personal care plan demonstrates how vital patient information can become invisible within hospital computerised records, leading directly to missed vital sign checks that could have prevented serious harm.
Your IT systems are making it very difficult or impossible for clinicians to find critical information when they need it most. Clinical information is being buried within complex system architectures where your healthcare professionals cannot easily locate essential patient data during time-sensitive medical situations. This problem isn't just about poor user interface design – it's about fundamental flaws in how your healthcare software portals organize and present life-critical information.
The systematic nature of this problem means your clinicians are spending valuable time searching for information that should be immediately accessible. Your current healthcare software architecture treats all patient information with equal priority, failing to highlight or prominently display the most critical data points that could prevent patient harm. This information burial creates dangerous gaps in patient care continuity.
System failures preventing medication tracking and dosing
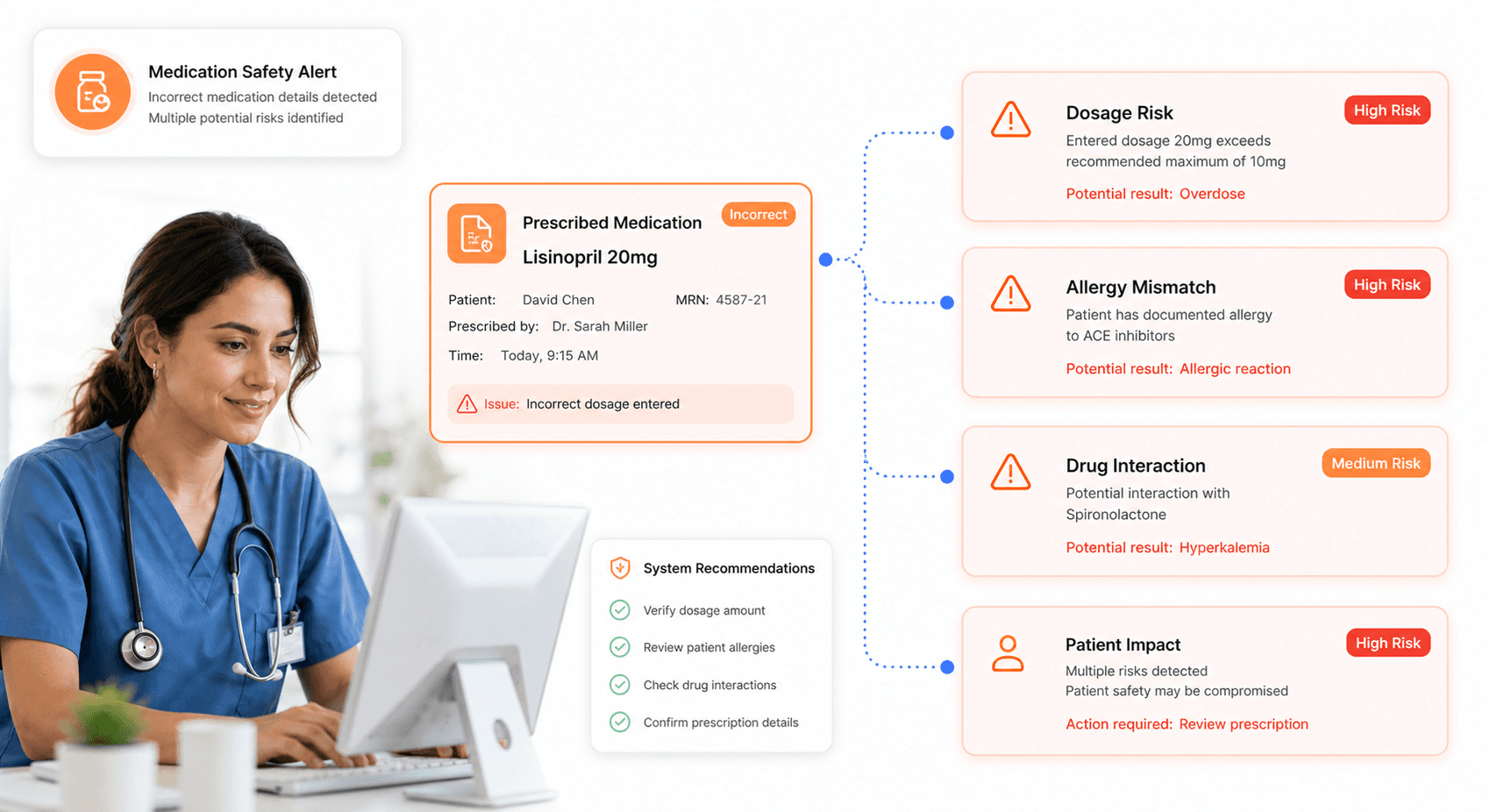
Your healthcare software portals are experiencing critical system failures that directly impact medication safety and patient outcomes. Medication errors and missed doses of antibiotics are occurring because your IT systems cannot reliably track and manage pharmaceutical interventions. These failures represent some of the most dangerous technical problems affecting patient safety within NHS digital infrastructure.
Your current systems are generating incorrect patient details on theatre lists, leading to wrong operations being scheduled or performed. The software failures extend to critical safety information, with incorrect allergy statuses being displayed or failing to display altogether. These medication tracking failures create scenarios where your patients receive inappropriate treatments that could cause severe adverse reactions or treatment failures.
The scope of medication-related system failures in your healthcare software portals indicates fundamental problems with data integrity and real-time information management. Your clinical teams are working with systems that cannot guarantee accurate, up-to-date medication information, forcing them to rely on manual verification processes that introduce additional opportunities for human error. These systematic medication tracking failures demonstrate why NHS IT failures continue to generate significant patient complaints and safety concerns.
Real-World Patient Harm Cases from NHS IT Failures
Deaths linked to inaccessible care plans and vital sign monitoring gaps
When your healthcare software portals fail to display critical patient information clearly, the consequences can be fatal. The tragic case of Darnell Smith demonstrates just how devastating NHS IT failures can be for patient safety. At only 22 years old, Smith died from pneumonia after hospital staff missed over 12 hours of vital sign checks. The root cause wasn't medical negligence, it was your Electronic Patient Record system's inability to make his personal care plan easily visible to the medical team.
This case highlights a fundamental flaw in how your healthcare software presents life-critical information. When care plans aren't prominently displayed or easily accessible within your computerised records, healthcare professionals may unknowingly overlook essential monitoring protocols. Your system's user interface design directly impacts whether patients receive the continuous care they need, and in Smith's case, this design failure proved fatal.
Delayed emergency treatment due to unclear patient prioritization systems
Your NHS software's inability to clearly identify and prioritize critically ill patients is creating dangerous delays in emergency treatment. Emily Harkleroad's death at age 31 serves as a stark reminder of these systemic failures. She died due to errors and delays in receiving urgent blood-thinning treatment because your new computer system failed to clearly highlight her critical status to medical staff.
This incident reveals a critical weakness in how your healthcare software portals handle patient prioritization. When your systems don't effectively communicate which patients require immediate attention, healthcare professionals struggle to make informed decisions about treatment urgency. The lack of clear visual indicators or priority flags in your electronic patient records means that time-sensitive treatments may be delayed, putting vulnerable patients at serious risk.
Over 200,000 unsent medical letters affecting patient care continuity
Your NHS computer systems have created a massive communication breakdown that's affecting hundreds of thousands of patients. A Freedom of Information request revealed that 200,000 medical letters went unsent across 21 trusts due to widespread NHS computer system problems. This isn't a minor administrative hiccup—it's a systemic failure that's disrupting the entire continuum of patient care.
When your healthcare software portals fail to send these critical communications, you're creating a cascade of problems that ripple throughout the healthcare system. Patients miss vital appointments because they never received notification letters. Cancer diagnoses are delayed when follow-up letters don't reach patients or their GPs. Medication changes go uncommunicated, potentially leading to dangerous drug interactions or continued use of inappropriate treatments.
These unsent letters represent broken links in your patient care chain, where each missing communication potentially compromises patient outcomes and safety.
More than 126 serious harm incidents across NHS trusts
The scope of NHS IT failures extends far beyond individual cases to reveal a pattern of systematic problems across your healthcare network. Freedom of Information requests have uncovered 126 instances of serious harm linked to IT issues across 31 trusts, with three deaths across two trusts directly related to Electronic Patient Record problems.
At Durham trust alone, your new IT system has been connected to over 2,000 incidents of potential patient harm. This staggering number demonstrates that your healthcare software portals aren't just experiencing isolated technical glitches, they're creating widespread safety risks that affect thousands of patients.
These incidents represent a fundamental breakdown in how your NHS digital transformation is being implemented and managed, showing that current healthcare software systems are consistently failing to meet the basic safety standards that patients deserve.
User Experience Issues Driving Patient Complaints
Multiple Portal Identities Created Across Different NHS Trusts
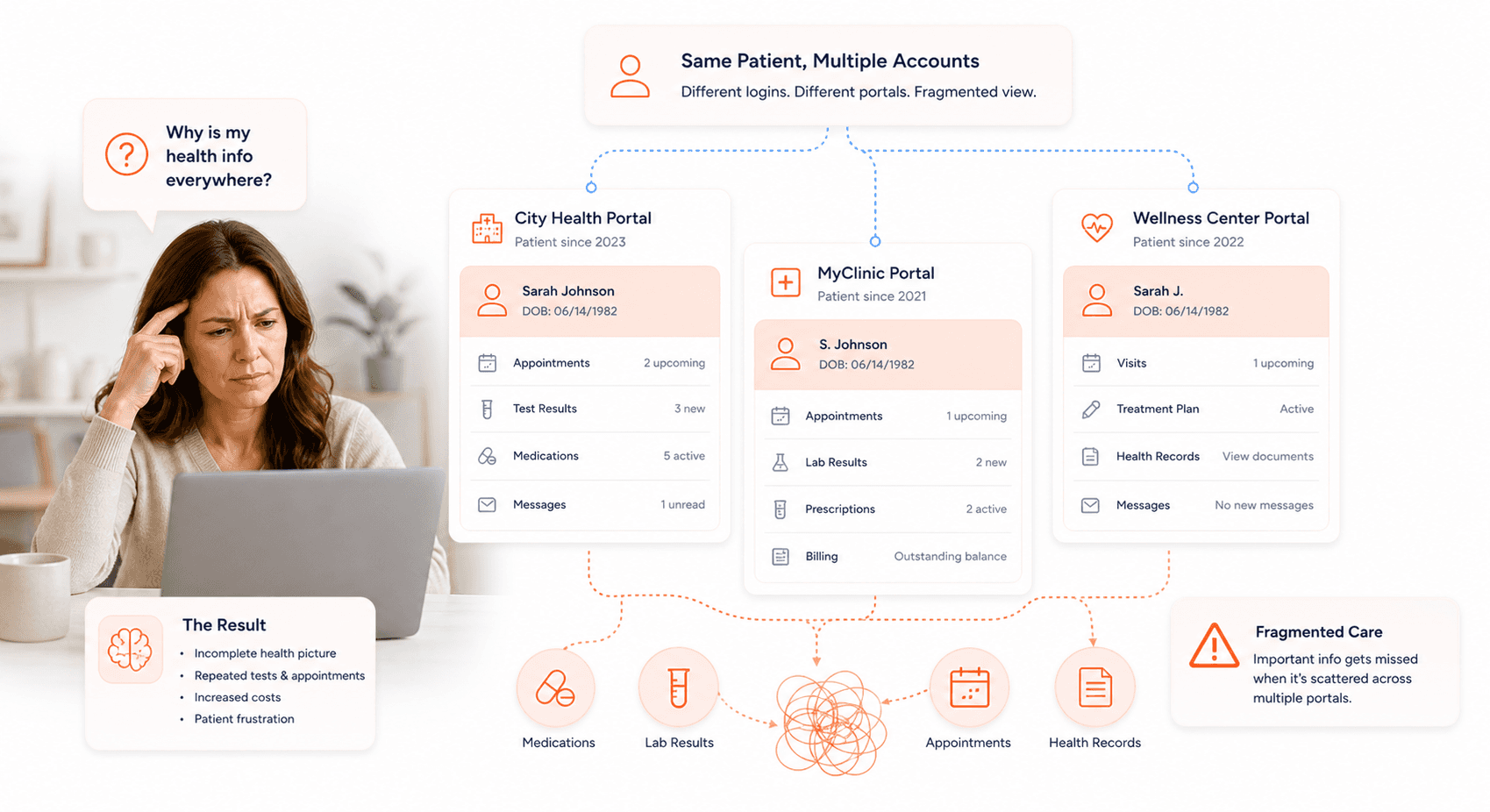
When you interact with NHS healthcare services across different trusts, you'll likely encounter one of the most frustrating aspects of the current healthcare software portal system: multiple identities for the same patient. Your experience navigating NHS digital services becomes unnecessarily complicated when each trust generates separate MyChart identities, creating a fragmented digital healthcare journey that compromises both efficiency and patient safety.
This duplication occurs because different NHS trusts operate independently with their own licensing agreements for systems like Epic's MyChart. As a patient, you might find yourself juggling multiple login credentials, different portal interfaces, and separate medical records despite being the same person receiving care within the same national health system. This fragmentation directly contributes to healthcare software portal complaints as you struggle to maintain a coherent view of your medical history across different healthcare providers.
The implications extend beyond mere inconvenience. When you have multiple portal identities, your healthcare providers may not have access to your complete medical history during critical care decisions. This creates potential NHS patient safety risks as important medical information becomes siloed across different systems, potentially leading to medication errors, missed allergies, or incomplete treatment plans.
Confusing Medical Data Presentation for Non-Medical Users
Your frustration with NHS electronic health records often stems from how medical information is presented within these healthcare software portals. The current systems display medical charts in formats designed for healthcare professionals, not patients seeking to understand their own health information. When you access your medical records through these portals, you're confronted with technical terminology, abbreviated codes, and clinical data formats that require medical training to interpret effectively.
This poor user experience design in NHS software systems increases your anxiety, particularly when reviewing test results or medical findings before GP appointments. Rather than providing clarity about your health status, these confusing presentations can lead to misunderstandings and unnecessary worry. The medical charts fail to translate complex clinical information into patient-friendly language, creating barriers to informed healthcare participation.
Your experience with these healthcare IT system failures reflects broader NHS digital transformation issues where system design prioritizes clinical workflows over patient usability. The result is electronic patient records that technically function for healthcare providers but fail to serve patients effectively, contributing to the growing number of healthcare software quality issues reported across the NHS.
Inadequate Helpdesk Support from NHS Trusts
When you encounter problems with these patient portal technical problems, your path to resolution becomes another source of frustration. You'll face significant challenges getting through to helpdesks operated by NHS trusts that license these systems. The support infrastructure often lacks adequate resources to handle the volume of patient inquiries, leaving you waiting extended periods for assistance with basic portal access or data correction issues.
Your experience with NHS helpdesk services reveals systematic underfunding and understaffing of patient support functions. These support limitations compound the existing usability problems, creating a cycle where poor system design generates support requests that cannot be adequately addressed. This inadequate support structure particularly impacts vulnerable patient populations who may require additional assistance navigating digital healthcare services.
Low Patient Digital Literacy Creating Access Barriers
Your ability to effectively use these healthcare software portals is further compromised by the assumption that all patients possess adequate digital literacy skills. The current NHS electronic health records systems require navigation skills, technical understanding, and comfort with digital interfaces that many patients lack. This digital divide creates significant access barriers, preventing you from fully utilizing available healthcare services and contributing to health inequalities.
Low patient digital literacy around products like MyChart creates user difficulties that extend beyond simple technical challenges. You may struggle with password management, understanding privacy settings, or interpreting system notifications, all of which can impact your healthcare engagement. These healthcare software user experience problems disproportionately affect older patients and those from disadvantaged socioeconomic backgrounds, creating additional barriers to equitable healthcare access.
Systematic Problems with NHS Electronic Patient Records
Lack of connectivity between different trust systems
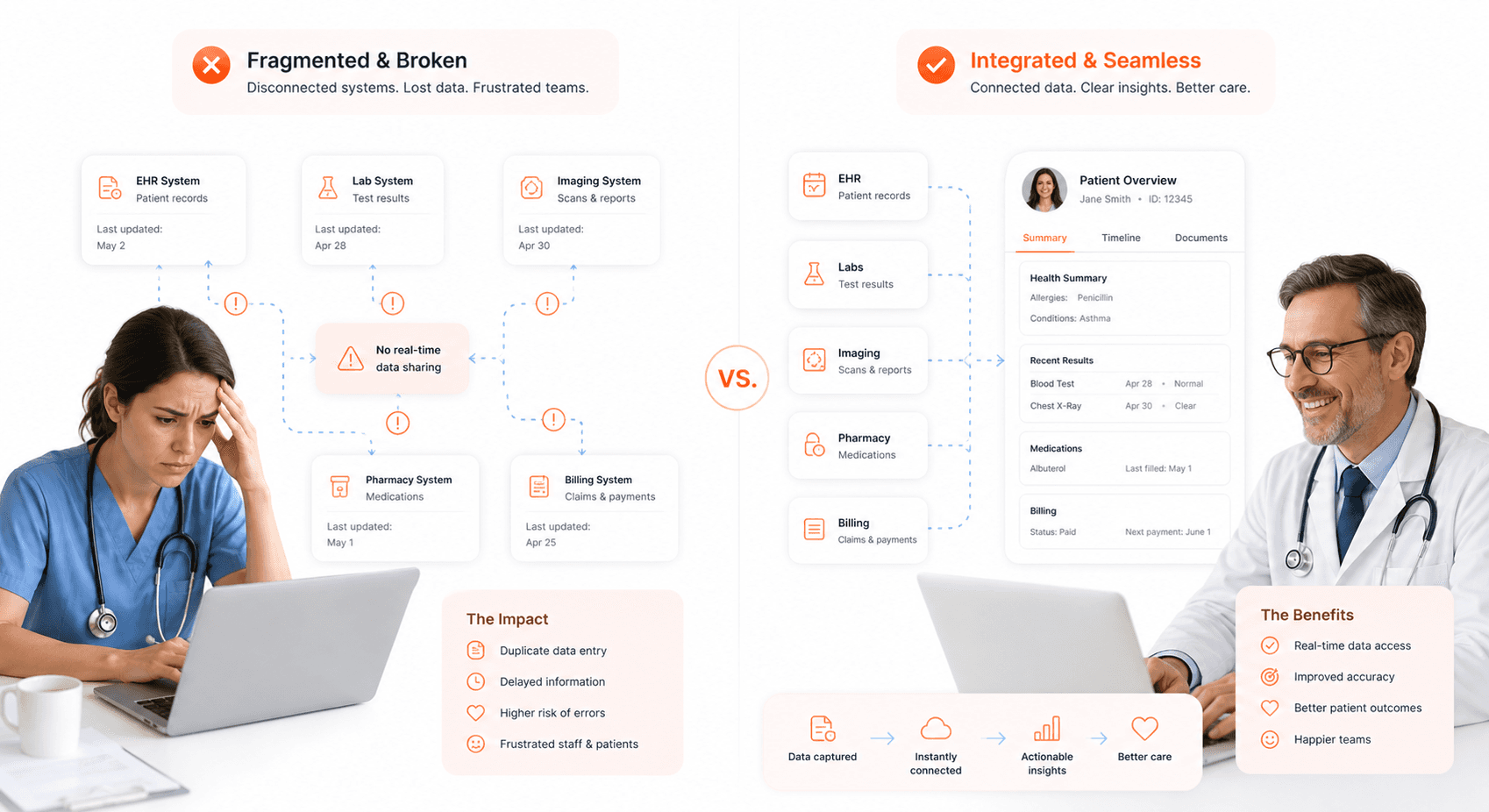
Your NHS electronic patient records system faces a fundamental challenge that undermines its core purpose: the complete lack of connectivity between different trust systems. This fragmentation creates what healthcare experts describe as a "broken jigsaw," where very few systems can communicate with each other effectively. When you're trying to access patient information across different NHS trusts, you'll encounter significant barriers that prevent seamless information sharing.
This connectivity crisis means that when your patients move between different healthcare providers or require specialist care at another trust, their electronic health records don't follow them. You're left struggling with incomplete patient histories, missing critical medical information, and potential gaps in care continuity. The fragmented access to secondary care compounds these problems, making it difficult for you to provide comprehensive patient care when referrals and specialist consultations are needed.
Your current NHS electronic patient records infrastructure operates as isolated islands rather than an integrated network. This lack of interoperability forces you to rely on manual processes, phone calls, and paper-based systems to share vital patient information between trusts. The result is delayed care decisions, increased administrative burden, and heightened risks of medical errors due to incomplete patient records.
Inadequate clinician input during system design and implementation
Your healthcare software portals suffer from a critical flaw: they're designed without adequate input from the clinicians who must use them daily. This fundamental oversight in system development means that your NHS IT failures often stem from solutions that don't align with real-world clinical workflows and requirements.
When you're working with electronic patient records that weren't designed with clinician input, you face systems that are unreliable and ineffective for actual patient care. The disconnect between software functionality and clinical needs creates barriers to efficient healthcare delivery. Your daily workflow becomes disrupted by systems that require workarounds, consume excessive time, or fail to support critical care decisions.
The absence of meaningful clinician involvement during design and implementation phases results in healthcare software that prioritizes technical specifications over practical usability. You're forced to adapt your clinical practice to accommodate poorly designed systems rather than having technology that enhances your ability to provide quality patient care.
Financial pressures leading to rushed deployments
Your NHS digital transformation faces enormous financial pressures that directly impact the quality and effectiveness of electronic patient records implementations. The huge financial costs associated with these systems create pressure for rapid deployments, often at the expense of thorough testing and proper system optimization.
When you're dealing with rushed deployments driven by budget constraints, your healthcare software portals are more likely to experience technical problems and user experience issues. These financial pressures force trusts to implement systems before they're ready for live clinical environments, leading to the patient safety risks and healthcare IT system failures that generate complaints.
Your trust's need to show return on investment quickly conflicts with the time required for proper system implementation. This tension results in healthcare software quality issues that could have been prevented with adequate deployment timelines and resources.
Limited ability to make urgent system adaptations
Your current NHS electronic health records infrastructure lacks the flexibility to respond quickly when problems are identified. This limitation in making urgent system adaptations means that when you discover critical issues affecting patient care or safety, you're unable to implement necessary fixes promptly.
The rigid nature of your healthcare software systems creates a dangerous situation where known problems persist because the infrastructure cannot accommodate rapid changes. When you identify patient portal technical problems or discover flaws that impact clinical decision-making, the lengthy process required for system modifications can leave these issues unresolved for extended periods.
Your ability to provide safe, effective patient care is compromised when the technology supporting your work cannot be quickly adapted to address emerging problems or changing clinical requirements.
Hidden Scale of NHS IT Problems and Cover-Up Culture
Nearly Half of Hospital Trusts Reporting Patient-Affecting IT Issues
The scope of NHS IT failures affecting your patient care extends far beyond isolated incidents. Recent investigations reveal that nearly half of hospital trusts with electronic patient systems have reported issues that could directly affect your safety and treatment outcomes. This staggering statistic represents a systemic failure that puts your wellbeing at risk every time you interact with NHS healthcare software portals.
When you consider that almost half of trusts have recorded instances of potential patient harm linked to their systems, the implications for your healthcare experience become deeply concerning. Nearly 60 trusts have specifically reported IT problems affecting patient care, meaning your medical records, treatment plans, and diagnostic information could be compromised by faulty healthcare software systems. These NHS IT failures aren't merely technical inconveniences - they represent direct threats to your patient safety and care quality.
Reluctance of Clinicians to Speak Publicly About System Failures
Your healthcare providers are witnessing these NHS software user experience problems firsthand, yet a concerning pattern of silence prevents you from understanding the true scope of these issues. When BBC News contacted clinicians about electronic patient records problems, they discovered that healthcare professionals did not want to be named due to fears over speaking out about system failures.
This reluctance creates a dangerous information gap that directly affects your ability to make informed decisions about your healthcare. Your doctors, nurses, and other healthcare providers may be struggling with malfunctioning healthcare IT system failures daily, but institutional pressure prevents them from publicly discussing how these issues impact your care. This culture of silence means you remain unaware of the technical problems that could be affecting your treatment outcomes and medical record accuracy.
Comparison to Post Office Horizon Scandal Patterns
Your situation as an NHS patient bears troubling similarities to the victims of the Post Office Horizon scandal. Professor Joe McDonald has identified clear echoes between the Post Office scandal patterns and current NHS IT failures, suggesting that your complaints about healthcare software portal problems may be part of a much larger systemic issue.
Just as Post Office workers were blamed for system errors that weren't their fault, you may find your concerns about NHS digital transformation issues dismissed or minimized when the real problem lies with faulty electronic health records systems. This parallel should alarm you because it suggests that your patient portal technical problems aren't isolated incidents but symptoms of a broader institutional failure to acknowledge and address healthcare software quality issues.
Insufficient Transparency About System Problems and Patient Risks
Perhaps most concerning for your safety is the revelation that there is "undoubtedly a culture of cover-up in the NHS, and nowhere is that stronger than in the health IT sector." This culture of secrecy means you're not receiving transparent information about how healthcare software failures might be affecting your treatment.
An expert from Patient Safety Learning suggests that tens of thousands of serious issues involving patient harm or death due to these systems probably never get discussed. This means your experiences with problematic NHS healthcare software may be part of a much larger pattern of unreported incidents. The lack of transparency about these electronic patient records problems prevents you from fully understanding the risks you face when your healthcare relies on these failing systems.
Your right to safe, reliable healthcare is being compromised by this institutional reluctance to acknowledge the scope of NHS IT failures. Without proper transparency about healthcare IT system failures, you cannot make informed decisions about your care or hold the system accountable for improving your patient safety.
Current NHS Response and Investment Challenges
£900 million investment in new electronic patient record systems
Your healthcare organization is part of a massive financial commitment that NHS England has made to address ongoing IT challenges. Over the past two years, nearly £900 million has been invested specifically to help local organizations like yours introduce new and improved electronic patient record systems. This substantial investment reflects the scale of the problems you're experiencing with current healthcare software portals and the urgent need for comprehensive solutions.
When you examine this investment closely, you'll see it represents one of the largest commitments to healthcare IT infrastructure in NHS history. Your organization may have already received funding from this allocation, or you might be planning to apply for resources to upgrade your current systems. The sheer magnitude of this investment acknowledges that the NHS IT failures affecting your daily operations require significant financial resources to resolve effectively.
However, your experience with these investments may vary significantly depending on how well the funding translates into practical improvements. The money is specifically targeted at helping organizations move away from problematic legacy systems that have been generating the complaints you're dealing with regarding healthcare software portal issues and NHS patient safety risks.
Ongoing deadline extensions for paperless NHS goals
Your organization's digital transformation efforts are occurring within a broader context of repeatedly missed government targets. The government's ambitious goal for achieving a paperless NHS has seen its latest deadline extended to 2026, which clearly implies that previous deadlines have been missed. This pattern of deadline extensions directly impacts your planning and implementation strategies for addressing electronic patient records problems.
When you consider these延期 delays, you can understand why your current systems may still be causing the complaints you're receiving. The extended timelines suggest that the complexity of transitioning to fully digital healthcare operations is far greater than initially anticipated. Your organization is operating within a healthcare system that has consistently underestimated the time required to properly implement and optimize NHS electronic health records systems.
These deadline extensions also indicate that your current challenges with healthcare software quality issues are not unique to your organization. The systemic nature of these delays suggests that the problems you're experiencing with patient portal technical problems are part of a wider pattern affecting the entire NHS digital transformation process.
Gap between promised benefits and actual system performance
Your daily experience with electronic patient record systems likely reflects a significant disconnect between what was promised and what you're actually receiving. Despite claims from system providers that access to medical records helps patients and makes healthcare more efficient, users like yourself report that these systems cause as many problems as they solve. This gap between promise and reality explains many of the NHS software user experience complaints you're encountering.
When you evaluate your current systems against the marketing promises that were made during procurement, you'll likely find substantial differences in performance, usability, and reliability. The providers assured you that these systems would streamline operations, reduce errors, and improve patient outcomes. However, your real-world experience may include system downtime, difficult navigation interfaces, and integration issues that actually hinder rather than help your healthcare delivery.
Your staff members are probably experiencing frustration because they were told these systems would make their jobs easier, yet they're finding themselves spending more time navigating complex interfaces and dealing with technical issues. This disconnect contributes directly to the healthcare IT system failures that generate patient complaints about service delays and access problems.
Need for improved safety standards and oversight protocols
Your organization operates within a system where NHS England acknowledges that electronic patient record systems can improve safety and care, particularly by helping clinicians detect conditions like sepsis. However, the critical safety risks associated with poor implementation and oversight cannot be ignored. Coroners have issued stark warnings about a "real risk of further deaths" if doctors cannot access important patient information when they need it most.
When you implement or upgrade your systems, you must recognize that there is an essential need for these systems to be introduced and operated to high standards. NHS England is working with trusts to review concerns and provide support on safe system use, but your organization bears primary responsibility for ensuring patient safety during this transition period.
Your oversight protocols must address the fundamental tension between the potential benefits of digital systems and the real risks they pose when implemented poorly. The safety standards you establish need to account for system failures, backup procedures, and staff training requirements that go far beyond basic technical competency.
Conclusion
The evidence is clear: NHS healthcare software portals are causing significant patient safety risks and complaints due to fundamental technical failures, poor user experience design, and systemic implementation problems. With IT system failures linked to patient deaths, over 200,000 unsent medical letters, and widespread reports of serious harm across hospital trusts, you cannot afford to ignore these critical issues. Your current electronic patient record systems may be creating more problems than they solve, particularly when staff cannot access vital patient information or when technical glitches prevent proper care coordination.
If you're responsible for NHS IT systems, you must prioritize immediate action to address these safety concerns before more patients are harmed. The £900m NHS investment in new systems will only be effective if you ensure proper integration, comprehensive staff training, and robust safety protocols. Your patients deserve healthcare technology that enhances rather than endangers their care - and that means demanding better from your software providers, implementing thorough testing protocols, and maintaining transparent reporting of system failures. The time for cover-ups and delayed responses has passed; patient safety must come first in every IT decision you make.

About the author
I’m the founder of Hashbyt, an AI-first frontend and UI/UX SaaS partner helping 200+ SaaS companies scale faster through intelligent, growth-driven design. My work focuses on building modern frontend systems, design frameworks, and product modernization strategies that boost revenue, improve user adoption, and help SaaS founders turn their UI into a true growth engine.
Is a clunky UI holding back your growth?
Is a clunky UI holding back your growth?
▶︎
Transform slow, frustrating dashboards into intuitive interfaces that ensure effortless user adoption.
▶︎
Transform slow, frustrating dashboards into intuitive interfaces that ensure effortless user adoption.